Testicular Cancer – Educational Information and Resources
Testicular cancer treatment in Delhi NCR. Gold Medalist (AIIMS), formerly at AIIMS New Delhi for more than 12 years. Testicular cancer is one of the most curable cancers where around 95% of patients can expect to be completely cured of their illness. भारत दिल्ली में टस्टेस (आदमी की गोलियां) के कैंसर का पक्का इलाज. Access world class treatment of testicular cancer in Delhi, Gurgaon, Noida, Ghaziabad with testicular cancer immunotherapy, chemotherapy, surgery and bone marrow transplantation. More information here
Call/Whatsapp: +919013812875

Receiving the Gold Medal for best Medical Oncologist AIIMS New Delhi
What is testicular cancer?

A testicular cancer specimen, cut open to show details. Photo courtesy wikimedia
Cells of the body normally divide to produce new cells. This division is normally tightly controlled, and stops when enough cells are produced.
Cancer is a disease when some cells of the body become abnormal and start dividing uncontrollably. Also, these damaged cells gain the ability to spread to distant sites of the body. When cancer affects the testes (the male reproductive organs), it is called testicular cancer.
Learn more about cancer and why it occurs
What age group does testicular cancer occur in?
Testicular cancer is a disease of adolescents and young boys. The typical age group for the vast majority of cases is men between 15 and 45. In fact, it is the most common cancer to occur among boys and men of the age group 15-35 years. However, it may be seen at any age.
Are there any risk factors for testicular cancer?
There are a few risk factors for testicular cancer as follows:
- A person whose testes have not descended into his scrotum (cryptoorchidism) has a 1% lifetime risk of developing testicular cancer. An oncologist or urological surgeon should be consulted for treatment of the same.
- A person who has had testicular cancer in one testis has an increased risk of testicular cancer in the contralateral testis
- As discussed below, there is a strong familial predisposition associated with testicular cancer. If a person’s father or brother has had testicular cancer, his risk of developing testicular cancer is increased.
Someone in my family has had testicular cancer, does that increase my risk?
Yes. As mentioned above, testicular cancer in one’s father or brother increases his risk of developing testicular cancer. Increased alertness for a testicular lump is warranted in these people.
Can testicular cancer spread from one person to another?
Testicular cancer is not contagious and cannot spread to another person by any method, including air, water, urine or semen.
What does “germ cell tumor” (GCT) mean?
Germ cell tumor refers to the most common type of testicular cancer (comprising the vast majority). Germ cells are cells that normally divide to produce sperm cells inside the testes. When these cells undergo mutations and transform into testicular cancer, these are called germ cell tumors of the testes.
Germ cell tumors of the testes are divided into the following main categories:
- Seminoma – these are about half of all tumors, usually occur in older patients, and are usually easier to treat
- Non-seminomatous germ cell tumors (NSGCT) – These generally occur in younger boys, and require more therapy than seminomas. Some subtypes include:
- Teratomas
- Embryonal carcinoma
- Choriocharcinoma
- Yolk Sac Tumor
- Mixed NSGCT
Are there other testicular cancers besides germ cell tumors?
Yes! There are more than a dozen different type of cancers that can arise from the testes. The vast majority are germ cell tumors (as discussed above). Uncommonly, testicular cancers can be:
- Lymphomas: These generally occur in older men, around 60 years of age
- Paratesticular rhabdomyosarcomas: Generally seen in children or young boys
- Very rarely, other subtypes
What is a teratoma?
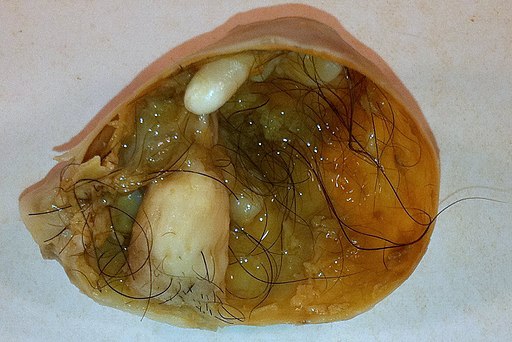
An opened teratoma showing various tissues, hair and teeth. Image courtesy Ed Uthman, USA
A teratoma is a special kind of testicular germ cell tumors where different normal body structures like hair, teeth, nervous tissue, cartilage and skin can develop inside the tumor. Although these tumors often look frightening, they are generally curable just like other NSGCTs.
Teratomas can also occur in females (ovarian teratomas) or mediastinum/retroperitoneum of both genders.
What are the common symptoms of testicular cancer?
The vast majority of testicular cancers are detected when the patient finds a lump in his testis. The lump can be painless (usually) or painful (sometimes).
If the testicular cancer spreads, it can lead to additional symptoms like…
- Pain in the abdomen or pelvis
- Swellings in the abdomen or inguinal area
- Blood in sputum, breathlessness or chest pain
In advanced stage, testicular cancer can spread anywhere in the body, but the vast majority spread within the abdomen or to the lungs.
Is a lump/mass in the testes always cancer?
Not at all! A lump in the testis can be due to various benign processes (such as infection, fluid collection, venous engorgement, cysts etc). An expert oncologist/urologist can guide you regarding the ideal treatment of a testicular lump.
Obtain expert surgical (urologist) opinion regarding a testicular lump
Oncological opinion on testicular cancer – free e-consultation
What tests are generally required before testicular cancer treatment in Delhi?
The first test done is almost always a testicular ultrasound. An ultrasound can determine if a testicular swelling is suspicious for cancer with a high level of certainty. In case of suspicion for testicular cancer, generally the following tests are done (all tests not needed in every patient):
- CT scanning of the abdomen, pelvis and chest
- Blood tests including tumor markers (see below)
- Surgical removal of the testis
- Additional tests in selected patients
Does testicular cancer lead to infertility? My semen testing was done before cancer treatment and it is abnormal…
It has been noted that due to abnormal function of the testis and hormones produced by testicular cancer, about 60-80% of patients have some abnormalities in semen at the time of diagnosis. These abnormalities usually resolve with treatment.
I wish to have children in future, can this be ensured?
Patients who receive chemotherapy or radiotherapy may develop infertility in 30-40% of cases. Therefore, men who wish to have children in the future should have their semen preserved for future use. This factor should always be discussed with your oncologist.
Ask a question about fertility and chemotherapy
What are tumor markers? What is hCG, AFP and LDH?
hCG (human chorionic gonadotropin), AFP (Alpha fetoprotein) and LDH (Lactate dehydrogenase) are substances that are normally present in the blood in very small amounts. In testicular cancer, the levels of these substances often increase to large amounts, thus these are called “tumor markers”.
Tumor markers are useful for diagnosis, monitoring treatment, and follow up of testicular cancer.
Can we do biopsy from testis to confirm the diagnosis of testicular cancer?
Unfortunately, removal of the diseased testis is considered mandatory for complete cure of testicular cancer in most cases. Also, biopsy carries the risk of spreading of cancer along the biopsy tract. Therefore, testicular biopsy is generally not done and instead the whole testis is removed by surgery, a process called orchiectomy.
Consult an expert urological surgeon for orchiectomy
What are the stages of testicular cancer?
Testicular cancer generally has 3 stages. This is different from most other cancers which have 4 stages, and is because testicular cancer has a high cure rate at every stage. Thus stage 4 testicular cancer does not exist.
Roughly, the stage division is as follows:
Stage IA/IB: Cancer confined to the testis
Stage IS: Cancer spread beyond the testis but not visible on CT
Stage II: Cancer spread beyond the testis into the abdomen, with markers that are not highly elevated
Stage III: Cancer spread beyond the abdomen or cancer within the abdomen with very high markers
How is testicular cancer generally treated?
The vast majority of testicular cancers are treated with a combination of:
- Surgery, to remove the cancerous testis and other sites of disease
- Chemotherapy, to eliminate cancer from sites which are difficult to operate or not visible on CT scanning
What is chemotherapy? How successful is it in treating testicular cancer?
Testicular cancer is highly sensitive to chemotherapy
Testicular cancer is one of the most chemosensitive cancers in the world. Chemotherapy is so effective in testicular cancer that the prognosis of stage III cancer has improved from nearly zero in the pre-chemotherapy era to more than 80% today. This entire improvement can be attributed to the effectiveness of modern chemotherapy.
Learn more about chemotherapy in testicular cancer
Is testicular cancer chemotherapy safe?
In skilled hands, testicular cancer chemotherapy is generally considered very safe. Side-effects do occur but serious side-effects that threaten life are rare. Most fit patients complete their chemotherapy without facing any dangerous side-effects. Careful treatment by an expert medical oncologist is mandatory to achieving a good outcome.
Learn more about chemotherapy and its side effects
Access Dr Vineet’s detailed CV
How many cycles of chemotherapy are needed to cure testicular cancer?
The number of cycles varies from stage to stage. In general, stage I patients do well either without chemotherapy or require 1-2 cycles. Stage II-III patients generally require 3-4 cycles depending upon the exact stage.
Uncommonly, patients who do not respond well to frontline chemotherapy and require additional chemotherapy (see relapsed disease below).
Why is testicular cancer called “a highly curable cancer”? What is the cure rate (successful treatment rate) for testicular cancer?
Testicular cancer is generally considered one of the “miracles” of modern oncology. In the advanced stage, this is a cancer which was incurable and led to certain death in the prechemotherapy era. Currently, around 80% of Stage III patients get cured. Cure statistics for testicular cancer by stage are as follows:
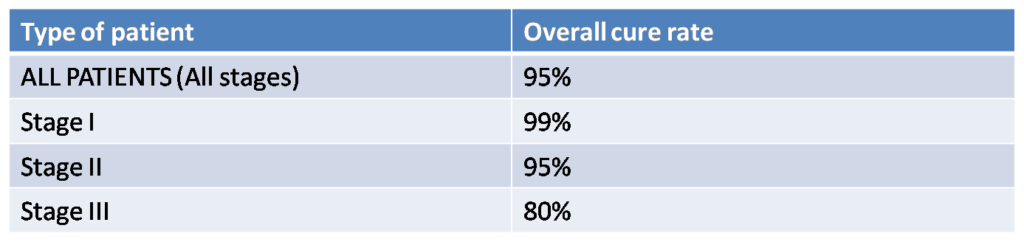
Cure rate of testicular cancer at various stages
These figures are continuously improving and in a decade or two, a 99-100% cure rate may not be unrealistic at every stage.
Cancer is a curable disease! Learn more
My doctor tells me there is no longer any cancer in my body! Do I still need to get tested?
Once testicular cancer is fully treated (no cancer in body) there is a small risk of relapse (disease coming back). If testicular cancer does come back, it is important to catch it early and treat it before it leads to organ injury or increases to an incurable state. Thus, generally patients require 3-4 monthly doctor visits. blood tests and CT scans for the first 2-3 years after successful treatment. Thereafter, the frequency of follow up comes down to once in six months or once in a year.
What is relapsed or refractory testicular cancer? How is it treated?
Relapsed/refractory testicular cancer means cancer that either (1) fails to get cured with initial therapy or (2) comes back after initial therapy. Relapsed/refractory testicular cancer is curable. Treatment generally consists of chemotherapy, surgery and (sometimes) bone marrow transplantation.
What is bone marrow transplantation? When is it used for testicular cancer?
Bone marrow transplantation (BMT) is a procedure that involves:
- Eliminating the patient’s own hematopoietic (blood producing) and immune (infection fighting) system
- Replacing it with the patient’s own (autologous) or foreign (allogenic) system
In relapsed testicular cancer, BMT is used rarely for patients who cannot be cured by chemotherapy alone. However, because BMT is a major procedure and associated with many side-effects, risks and costs, it is not used in most patients and only in highly selected patients with aggressive, difficult to treat cancer.
What is cancer immunotherapy in testicular cancer? Is it helpful?

Immunotherapy is a new revolution in cancer
Immunotherapy is a new way of treating cancer that uses the body’s own immune system to attack cancer cells. Immunotherapy is not routinely used for testicular cancer, partly because chemotherapy is so successful in producing cures (see above). However, it has been applied experimentally to some patients who have failed other modalities of treatment.
The status of immunotherapy for testicular cancer is experimental as of 2017. Several trials are ongoing to define its role better.
Learn more about cancer immunotherapy
Why should I seek a cancer specialist for testicular cancer treatment in Delhi?
Testicular cancer is simultaneously highly aggressive and highly curable. If treated inappropriately or untreated, it can spread very rapidly and cause death in a matter of months in some cases. With proper treatment more than 95% of patients can be cured. Thus an expert medical oncologist can mean the difference between cure and death. This makes it essential that an expert medical oncologist is consulted for treatment of testicular cancer. Dr Vineet is a specialist in the treatment of testicular cancer in Delhi and is gold medalist from AIIMS New Delhi with 12+ years at AIIMS. You can get more information here. Access his detailed curriculum vitae here.
I need more information….
Information about cancer and various aspects of its treatment are available on this website. Some common queries are linked below. Others can be accessed by using the menu at the top of this page or the search box. If your question is not answered here you can send us a free e-consultation using the form below.
- General information about cancer
- Information about chemotherapy
- Information about targeted therapy
- Information about cancer immunotherapy
- Prostate cancer, another common reason for orchiectomy
- Kidney cancer, another common urological cancer
Free E-consultation for testicular cancer treatment in Delhi
Testicular cancer is an eminently curable cancer and multiple resources are available above for its treatment in Delhi. If you need more information you can use the below form or Email us at vineetgovindagupta@gmail.com or call/whatsapp at +919013812875
